Transition zone v2 v3. Electrocardiographic signs of myocardial hypertrophy. Biocurrents in the heart can be recorded
From this article you will learn about such a diagnostic method as ECG of the heart– what it is and what it shows. How an electrocardiogram is recorded, and who can most accurately decipher it. You will also learn how to independently determine the signs of a normal ECG and major heart diseases that can be diagnosed using this method.
Article publication date: 03/02/2017
Article updated date: 05/29/2019
What is an ECG (electrocardiogram)? This is one of the simplest, most accessible and informative methods for diagnosing heart disease. It is based on recording electrical impulses arising in the heart and graphically recording them in the form of teeth on a special paper film.
Based on these data, one can judge not only the electrical activity of the heart, but also the structure of the myocardium. This means that an ECG can diagnose many different heart conditions. Therefore, independent interpretation of the ECG by a person who does not have special medical knowledge is impossible.
All that an ordinary person can do is only roughly assess the individual parameters of the electrocardiogram, whether they correspond to the norm and what pathology they may indicate. But final conclusions based on the ECG conclusion can only be made by a qualified specialist - a cardiologist, as well as a therapist or family doctor.
Principle of the method
The contractile activity and functioning of the heart is possible due to the fact that spontaneous electrical impulses (discharges) regularly occur in it. Normally, their source is located in the uppermost part of the organ (in the sinus node, located near the right atrium). The purpose of each impulse is to travel along the nerve pathways through all parts of the myocardium, causing them to contract. When an impulse arises and passes through the myocardium of the atria and then the ventricles, their alternating contraction occurs - systole. During the period when there are no impulses, the heart relaxes - diastole.
ECG diagnostics (electrocardiography) is based on recording electrical impulses arising in the heart. For this purpose, a special device is used - an electrocardiograph. The principle of its operation is to capture on the surface of the body the difference in bioelectric potentials (discharges) that occur in different parts of the heart at the moment of contraction (in systole) and relaxation (in diastole). All these processes are recorded on special heat-sensitive paper in the form of a graph consisting of pointed or hemispherical teeth and horizontal lines in the form of spaces between them.

What else is important to know about electrocardiography
Electrical discharges of the heart pass not only through this organ. Since the body has good electrical conductivity, the strength of the exciting cardiac impulses is sufficient to pass through all tissues of the body. They spread best to the chest in the area, as well as to the upper and lower extremities. This feature is the basis of the ECG and explains what it is.
In order to record the electrical activity of the heart, it is necessary to fix one electrocardiograph electrode on the arms and legs, as well as on the anterolateral surface of the left half of the chest. This allows you to capture all directions of electrical impulses propagating throughout the body. The paths of discharges between the areas of contraction and relaxation of the myocardium are called cardiac leads and are designated on the cardiogram as follows:
- Standard leads:
- I – first;
- II – second;
- Ш – third;
- AVL (analogue of the first);
- AVF (analogue of the third);
- AVR (mirroring all leads).
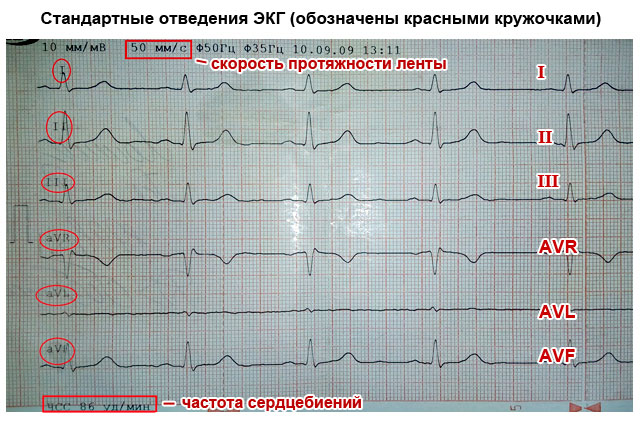
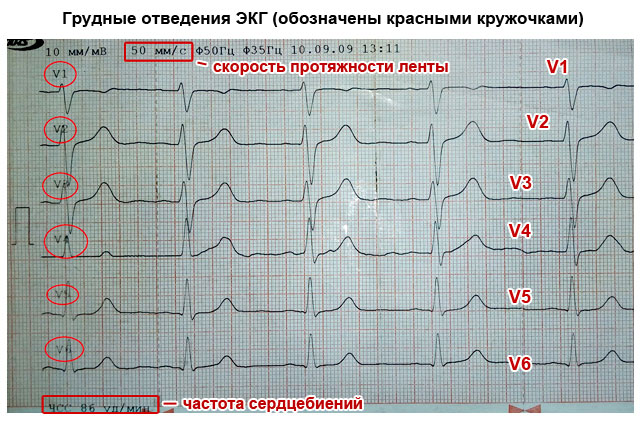
The significance of the leads is that each of them registers the passage of an electrical impulse through a certain area of the heart. Thanks to this, you can obtain information about:
- How the heart is located in the chest (the electrical axis of the heart, which coincides with the anatomical axis).
- What is the structure, thickness and nature of blood circulation of the myocardium of the atria and ventricles.
- How regularly do impulses occur in the sinus node and are there any interruptions?
- Are all impulses carried out along the paths of the conducting system, and are there any obstacles in their path?
What does an electrocardiogram consist of?
If the heart had the same structure of all its departments, nerve impulses would pass through them in the same time. As a result, on the ECG, each electrical discharge would correspond to only one tooth, which reflects the contraction. The period between contractions (impulses) on the EGC looks like an even horizontal line, which is called an isoline.
The human heart consists of right and left halves, in which the upper part is the atria, and the lower part is the ventricles. Because they have different sizes, thickness and are separated by partitions, the exciting impulse passes through them at different speeds. Therefore, different waves corresponding to a specific part of the heart are recorded on the ECG.

What do the teeth mean?
The sequence of propagation of systolic excitation of the heart is as follows:
- The origin of electric pulse discharges occurs in the sinus node. Since it is located close to the right atrium, it is this section that contracts first. With a slight delay, almost simultaneously, the left atrium contracts. On the ECG, such a moment is reflected by the P wave, which is why it is called atrial. It faces up.
- From the atria, the discharge passes to the ventricles through the atrioventricular (atrioventricular) node (a collection of modified myocardial nerve cells). They have good electrical conductivity, so delays in the node do not normally occur. This is displayed on the ECG as the P-Q interval - a horizontal line between the corresponding teeth.
- Excitation of the ventricles. This part of the heart has the thickest myocardium, so the electrical wave travels through them longer than through the atria. As a result, the highest wave appears on the ECG - R (ventricular), facing upward. It may be preceded by a small Q wave, the apex of which faces in the opposite direction.
- After the completion of ventricular systole, the myocardium begins to relax and restore energy potentials. On the ECG it looks like an S wave (facing down) - a complete lack of excitability. After it comes a small T wave, facing upward, preceded by a short horizontal line - the S-T segment. They indicate that the myocardium has fully recovered and is ready to make another contraction.



Since each electrode attached to the limbs and chest (lead) corresponds to a specific part of the heart, the same teeth look different in different leads - they are more pronounced in some, and less in others.
How to decipher a cardiogram
Sequential ECG interpretation in both adults and children involves measuring the size, length of the waves and intervals, assessing their shape and direction. Your actions with decryption should be as follows:
- Unfold the paper with the recorded ECG. It can be either narrow (about 10 cm) or wide (about 20 cm). You will see several jagged lines running horizontally, parallel to each other. After a short interval in which there are no teeth, after the recording is interrupted (1–2 cm), the line with several complexes of teeth begins again. Each such graph displays a lead, so it is preceded by a designation of which lead it is (for example, I, II, III, AVL, V1, etc.).
- In one of the standard leads (I, II or III) in which the R wave is the highest (usually the second), measure the distance between three successive R waves (R-R-R interval) and determine the average value (divide number of millimeters per 2). This is necessary to calculate the heart rate per minute. Remember that these and other measurements can be made with a millimeter ruler or by calculating the distance using an ECG tape. Each large cell on the paper corresponds to 5 mm, and each dot or small cell inside it corresponds to 1 mm.
- Assess the spaces between the R waves: are they the same or different? This is necessary in order to determine the regularity of the heart rhythm.
- Sequentially evaluate and measure each wave and interval on the ECG. Determine their compliance with normal indicators (table below).
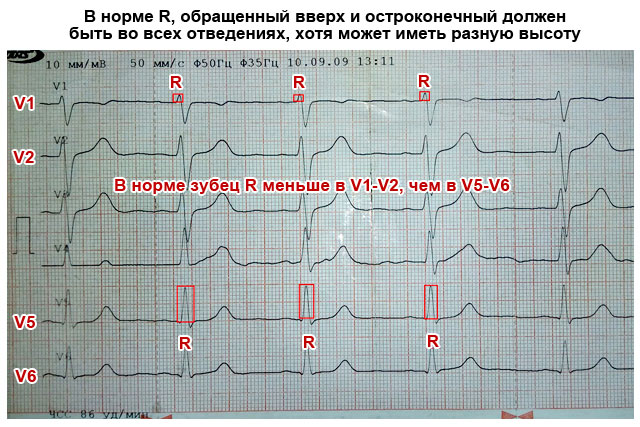
Important to remember! Always pay attention to the speed of the tape - 25 or 50 mm per second. This is fundamentally important for calculating heart rate (HR). Modern devices indicate heart rate on a tape, and there is no need to count.
How to count your heart rate
There are several ways to count the number of heartbeats per minute:
- Typically, the ECG is recorded at a speed of 50 mm/sec. In this case, you can calculate your heart rate (heart rate) using the following formulas:
Heart rate=60/((R-R (in mm)*0.02))
When recording an ECG at a speed of 25 mm/sec:
Heart rate=60/((R-R (in mm)*0.04)
- You can also calculate the heart rate on a cardiogram using the following formulas:
- When recording at 50 mm/sec: HR = 600/average number of large cells between R waves.
- When recording at 25 mm/sec: HR = 300/average of the number of large cells between the R waves.

What does an ECG look like normally and with pathology?
What a normal ECG and wave complexes should look like, what deviations occur most often and what they indicate are described in the table.
Important to remember!
- One small cell (1 mm) on the ECG film corresponds to 0.02 seconds when recording at 50 mm/sec and 0.04 seconds when recording at 25 mm/sec (for example, 5 cells - 5 mm - one large cell corresponds to 1 second).
- The AVR lead is not used for evaluation. Normally, it is a mirror image of standard leads.
- The first lead (I) duplicates the AVL, and the third (III) duplicates the AVF, so they look almost identical on the ECG.

| ECG parameters | Normal indicators | How to decipher deviations from the norm on a cardiogram, and what they indicate |
|---|---|---|
| Distance R–R–R | All spaces between R waves are equal | Different intervals may indicate atrial fibrillation, heart block |
| Heart rate | In the range from 60 to 90 beats/min | Tachycardia – when heart rate is more than 90/min Bradycardia – less than 60/min |
| P wave (atrial contraction) | Facing upward like an arc, about 2 mm high, precedes each R wave. May be absent in III, V1 and AVL | High (more than 3 mm), wide (more than 5 mm), in the form of two halves (double-humped) - thickening of the atrial myocardium |
| Generally absent in leads I, II, FVF, V2 – V6 – the rhythm does not come from the sinus node | ||
| Several small sawtooth-shaped teeth between the R waves – atrial fibrillation | ||
| P–Q interval | Horizontal line between P and Q waves 0.1–0.2 seconds | If it is elongated (more than 1 cm when recording 50 mm/sec) – hearts |
| Shortening (less than 3 mm) – | ||
| QRS complex | Duration is about 0.1 sec (5 mm), after each complex there is a T wave and there is a horizontal line gap | Expansion of the ventricular complex indicates hypertrophy of the ventricular myocardium, bundle branch block |
| If there are no gaps between high complexes facing upward (they go continuously), this indicates either ventricular fibrillation | ||
| Looks like a “flag” – myocardial infarction | ||
| Q wave | Downward facing, less than ¼ R deep, may be absent | A deep and wide Q wave in standard or precordial leads indicates acute or previous myocardial infarction |
| R wave | The highest, facing upward (about 10–15 mm), pointed, present in all leads | It may have different heights in different leads, but if it is more than 15–20 mm in leads I, AVL, V5, V6, this may indicate. A jagged R at the top in the shape of the letter M indicates a bundle branch block. |
| S wave | Available in all leads, facing down, pointed, can have different depths: 2–5 mm in standard leads | Normally, in the chest leads its depth can be as many millimeters as the height R, but should not exceed 20 mm, and in leads V2–V4 the depth of S is the same as the height of R. Deep or jagged S in III, AVF, V1, V2 – left ventricular hypertrophy. |
| Segment S–T | Corresponds to the horizontal line between the S and T waves | Deviation of the electrocardiographic line up or down from horizontal plane more than 2 mm indicates coronary disease, angina or myocardial infarction |
| T wave | Facing upwards in the form of an arc with a height of less than ½ R, in V1 it can have the same height, but should not be higher | A tall, pointed, double-humped T in the standard and chest leads indicates coronary disease and heart overload |
| The T wave merging with the S–T interval and the R wave in the form of an arcuate “flag” indicates an acute period of infarction |

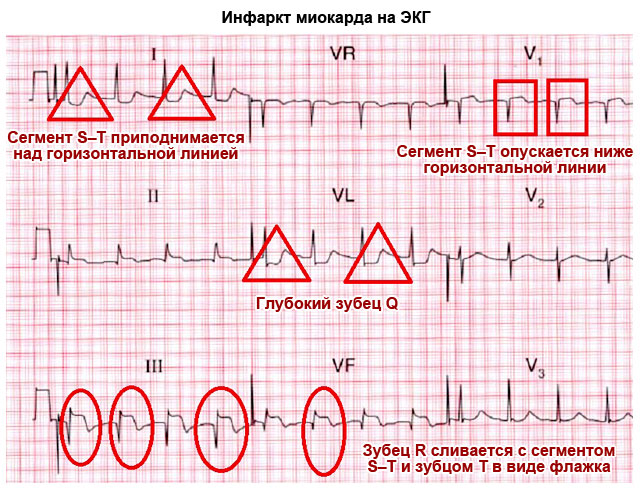
Something else important
The ECG characteristics described in the table in normal and pathological conditions are only a simplified version of the decoding. A full assessment of the results and the correct conclusion can only be made by a specialist (cardiologist) who knows the extended scheme and all the intricacies of the method. This is especially true when you need to decipher an ECG in children. The general principles and elements of the cardiogram are the same as for adults. But there are different standards for children of different ages. Therefore, only pediatric cardiologists can make a professional assessment in controversial and doubtful cases.
Marked deviations of the electrical axis of the heart from the norm are observed with ventricular hypertrophy and blockade of the branches of the His bundle.
Assessing the position of the electrical axis of the heart is difficult when the heart is rotated in the sagittal plane with the apex backwards, when there is a pronounced S wave in leads I, II and III.
To determine the position of the QRS vector in the horizontal plane, it is necessary to evaluate the ratio of the R and S waves in the chest leads. Normally, in lead V 1, the r wave has the smallest amplitude and the main wave is S. In leads V 2 -V 4, the amplitude of the R wave gradually increases, and the S wave decreases.
In lead V 4 (much less often in V 5), the R wave has its maximum height. In leads V 5 -V 6, the S wave usually disappears and a complex of the R or qR type is recorded, and the amplitude of the R wave is slightly reduced compared to V 4. In one of the chest leads, the R and S waves have the same amplitude. This point corresponds to the so-called transition zone.
In the transition zone, the myocardial potentials of the right and left ventricles are equal. Typically, this zone corresponds to the projection of the interventricular septum onto the anterior chest wall. Normally, the transition zone is usually located between V 2 and V4, more often in V 3. If the transition zone is located to the right of point V 3, then we talk about its shift to the right, and if it is to the left of position V 4, then it is said to shift to the left.
A shift of the transition zone to the left (to the region V 5) is possible with a vertical position of the heart, its rotation around the longitudinal axis clockwise (right ventricle forward) and with hypertrophy of the right ventricle; a shift of the transition zone to the right (towards V 1) may indicate a horizontal position of the heart, rotation around the longitudinal axis of the left ventricle forward or hypertrophy of the left ventricle.
Changes in the normal ratios of the amplitude of the R and S waves in the precordial leads can also be observed with infarctions and cicatricial changes in the myocardium, and various disorders of intraventricular conduction.
Wilson proposed a definition of the electrical position of the heart. A sign of a horizontal electrical position is the similarity of the shape of the QRS complex in leads aVL and V 5 -V 6, as well as in aVF and V 1 -V 2.
The vertical position is determined when the shape of the QRS complex is similar in leads aVL and V 1 -V 2, as well as aVF and V 5 -V 6. In addition, semi-horizontal, semi-vertical, intermediate and indefinite electrical position of the heart are distinguished. The diagnostic value of determining the electrical position of the heart is small, so at present this concept is practically not used.
“Practical electrocardiography”, V.L. Doshchitsin
Drug tests are performed to determine the cardiovascular system's response to various medications. During all tests, an ECG is recorded before and a certain time after using the drug. Research is carried out with the patient lying down, usually on an empty stomach. Atropine test To carry out this test, an ECG is recorded before and 15 and 30 minutes after subcutaneous administration of 1 ml of 0.1%...
When assessing the T wave, pay attention to its direction, shape and amplitude. As mentioned above, the T wave is usually directed towards the main wave of the QRS complex. Changes in the T wave are nonspecific and occur in a wide variety of pathological conditions. Thus, an increase in the amplitude of the T wave is possible with myocardial ischemia, left ventricular hypertrophy, hyperkalemia and is sometimes observed in ...

On a normal ECG, a number of waves and intervals between them are distinguished. There are P waves, Q, R and S waves, forming the QRS complex, T and U waves, as well as P-Q(P-R), S-T, Q-T, Q-U and T-P intervals. To characterize the relative amplitude of the Q, R and S waves, not only capital, but also lowercase letters q, r and s are used....
In children 3–14 years old, the electrical axis is within the range of +30° ÷ +70°. In children under 3 years of age, the electrical axis of the heart is in the sector +70° ÷ +100°.
Transition zone. When analyzing an ECG, the transition zone should be taken into account - it is determined by a lead in which the R and S waves are equiphase, i.e. their amplitude on both sides of the isoelectric line is equal. In healthy older children, the QRS transition zone is usually determined in leads V3,4. When the ratio changes vector forces the transition zone moves towards their predominance. For example, with right ventricular hypertrophy, the transition zone moves to the position of the left chest electrodes and vice versa. There is a gradual or abrupt formation of the transition zone. The transition zone has no independent significance in diagnosis. For example, with biventricular hypertrophy of the ventricular myocardium, no displacement of the transition zone is observed. However, in combination with other diagnostic signs, the displacement of the transition zone acquires a certain weight.
SI, II, III – ECG type. This designates an ECG that has an S wave in three standard leads, the amplitude of which is equal to or greater than the R amplitude, and a QRS complex of the RS form without a Q wave. In this case, there is often a low-voltage curve and rSRV1. This type of ECG occurs in a small number of observations (0.5 - 1%) in healthy children, relatively often in patients with pneumonia, with some congenital heart defects, etc. SI, II, III - type of ECG, caused by rotation of the heart around the transverse axis apex posteriorly. The diagnostic value of SI, II, III type ECG increases with its sudden appearance.
“Diseases of the heart and blood vessels in children”, N.A. Belokon
This information is for your information only; please consult your doctor for treatment.
Decoding a cardiogram in children and adults: general principles, reading the results, an example of decoding
Definition and essence of the method
How to correctly perform an electrocardiogram followed by
The principle of decoding an ECG
ECG interpretation plan - general scheme for reading results
- position of the electrical axis of the heart;
- determining the correctness of the heart rhythm and conductivity of the electrical impulse (blockades, arrhythmias are identified);
- determining the regularity of contractions of the heart muscle;
- determination of heart rate;
- identifying the source of the electrical impulse (whether sinus rhythm is determined or not);
- analysis of the duration, depth and width of the atrial P wave and the P – Q interval;
- analysis of the duration, depth, width of the QRST ventricular wave complex;
- analysis of parameters of the RS – T segment and T wave;
- analysis of Q – T interval parameters.
Based on all the studied parameters, the doctor writes a final conclusion on the electrocardiogram. The conclusion may roughly look like this: “Sinus rhythm with heart rate 65. Normal position of the electrical axis of the heart. No pathology was detected." Or this: “Sinus tachycardia with heart rate 100. Single supraventricular extrasystole. Incomplete blockade of the right bundle branch. Moderate metabolic changes in the myocardium."
If any of the 4 pathological syndromes are identified, then indicate which ones - rhythm disturbance, conduction, overload of the ventricles or atria, and damage to the structure of the heart muscle (infarction, scar, dystrophy).
Example of deciphering an electrocardiogram
Checking the regularity of heart contractions
Heart rate (HR) calculation
1. The speed of the tape is 50 mm/s - then the heart rate is 600 divided by the number of squares.
2. The speed of the tape is 25 mm/s - then the heart rate is 300 divided by the number of squares.
Identifying the source of the rhythm
Decoding ECG - rhythms
Detection of pathology of electrical impulse conduction through the structures of the heart
Electrical axis of the heart
Atrial P wave
- positive in I, II, aVF and chest leads (2, 3,4, 5, 6);
- negative in aVR;
- biphasic (part of the tooth lies in the positive region, and part in the negative) in III, aVL, V1.
The normal duration of P is no more than 0.1 seconds, and the amplitude is 1.5 - 2.5 mm.
1. Tall and sharp teeth in leads II, III, aVF appear with hypertrophy of the right atrium (“cor pulmonale”);
2. A P wave with two peaks and a large width in leads I, aVL, V5 and V6 indicates hypertrophy of the left atrium (for example, mitral valve disease).
P–Q interval
- I degree: simple lengthening of the P–Q interval while maintaining all other complexes and waves.
- II degree: prolongation of the P–Q interval with partial loss of some QRS complexes.
- III degree: lack of connection between the P wave and QRS complexes. In this case, the atria work in their own rhythm, and the ventricles - in their own.
Ventricular QRST complex
T wave
Q-T interval
ECG interpretation - normal indicators
5. Heart rate is 70 – 75 beats per minute.
6. sinus rhythm.
7. The electrical axis of the heart is located normally.
Interpretation of ECG in children and pregnant women
Decoding the electrocardiogram during a heart attack
The most acute stage of myocardial infarction can last for 3 hours - 3 days from the moment of circulatory disturbance. At this stage, the Q wave may be absent on the electrocardiogram. If it is present, then the R wave has a low amplitude or is completely absent. In this case, there is a characteristic QS wave, reflecting a transmural infarction. The second sign of an acute infarction is an increase in the S-T segment by at least 4 mm above the isoline, with the formation of one large T wave.
Interpretation of the most common ECGs
Also, myocardial hypertrophy can be a consequence of previous heart attacks.
Price of an electrocardiogram with interpretation
Read more:
Reviews
Heart rate..not clear 64 or 84
50mm\s 10 mm\mV 0.6-35; approximately 50 Hz Seconds: 1-5 Heart rate: 76 beats/min.
Please tell me the results are bad? What does it mean? I'm very worried(((thanks in advance
Leave feedback
You can add your comments and feedback to this article, subject to the Discussion Rules.
Transition zone v3 v4
Therefore, a small R wave is recorded in lead V1, and the presence of this wave is normal.
However, the main vector after excitation of the IVS is directed to the left, therefore, a negative wave is recorded in leads V1 and V2, namely the deep S wave.
V3 and V4. As the ventricles are covered by excitation, the EMF vector (main vector) directed to the left increases, therefore the height of the S wave in the leads V3 and V4 located to the left also increases.
The S1 wave, on the contrary, gradually decreases.
Often in lead V3 or V4, the R and S waves have equal amplitude.
These leads correspond to the so-called transition zone.
V5 and V6. The main vector of the EMF is directed towards leads V5 and V6, therefore the highest R waves are recorded in them. The T wave in leads V5 and V6 is positive.
We welcome your questions and feedback:
Please send materials for posting and wishes to:
By sending material for posting you agree that all rights to it belong to you
When quoting any information, a backlink to MedUniver.com is required
All information provided is subject to mandatory consultation with your attending physician.
The administration reserves the right to delete any information provided by the user
Normal ECG readings
Normal indicators of electrocardiogram elements.
P wave
- Normal duration:<120 мс.
- Height:<2,5 мм (≤2 мВ) – в стандартных отведениях, <1,5 мм (≤1мВ) – в грудных отведениях..
- Lead V1 is biphasic - negative phase width ≤40 ms and depth ≤1 mm
- Normally, there may be a slight splitting, usually in the chest leads. Distance between vertices<40 мс
- Always positive in I, II, V4-V6. Always negative in aVR.
- Best visualization in leads II and V1
- If it’s the other way around – dextrocardia, incorrect placement of electrodes on the arms, atrial rhythm.
- In aVF and V3 - usually positive, but may be biphasic or flattened.
- Variable: in III, aVL, V1-V2 - can be positive, negative and biphasic.
- The electrical axis of the tooth is located within the range from +30 to 75° in the frontal plane (exit beyond these limits may indicate the location of the pacemaker outside the sinus node).
PR interval
- Duration is normal (from the beginning of the P wave to the first wave of the QRS complex):
- In children -ms
- In adolescents -ms
- In adults – ms
- On average ms, 200 ms - at heart rate 40-50`, 150 ms at heart rate 80`
- Q wave: any initial negative deflection
- R wave: any positive deviation
- S wave: any negative deflection after the R wave
- Duration of the complex: ms, for the widest complex should not exceed 100 ms. If more than 100 ms – WPW syndrome or blockade of the legs of His.
- Amplitude of the QRS complex: MIN: in standard leads > 0.5 mV (0.5 cm), in V1-V6 > 1 mV (1 cm).
- The complexes are predominantly positive in I, II, aVF.
- The teeth are designated by capital letters (Q, R, S) with an amplitude of more than 3 mm.
- In the chest leads, the morphology of the QRS complex depends on the projection of the EMF vector onto the electrode.
- Internal deviation time: The distance from the first Q or R wave to the apex of the R wave in several precordial leads. The end of the internal deflection represents the moment the electrical impulse reaches the epicardial surface. For the right ventricle it is measured in leads V1 and V2 (upper limit 0.035), for the left ventricle - in leads V5 and V6 (upper limit 0.045).
EOS position
- From +90 to +180° - EOS deviation to the right.
- From -30 to -90° - EOS deviation to the left.
- From -90 to ±180° - extreme deviation of the EOS or deviation “up to the right”.
Standard options:
- In newborns - deviation to the right
- In childhood, the EOS is in a vertical position.
- Aged<40 лет – от 0 до +110°;
- At the age of >40 years – from -30° to +90°.
Q wave
Duration no more than 40 ms, depth no more than 2 mm and less than 25% of the subsequent R wave. Non-pathological Q waves are often observed in leads I, III, aVL, small q waves should always be present in V5 and V6.
- In leads V2-V4, the Q wave is wide<30 мс и глубиной >2 mm is considered pathological if the initial r wave (R) is observed in lead V1 and there is no noticeable shift of the transition zone to the right or left.
- In leads V2-V6, small Q waves may occur at extreme degrees of counterclockwise rotation (qR complexes)
- Aged< 30 лет глубина может достигать 5 мм в нескольких отведениях
- If in II, III, aVF the Q waves have borderline dimensions, width ≤ 30 ms and depth ≤ 4 mm, then they should be considered as: 1) leads with lower localization of Qs or 2) comparison with clinical data is required: borderline ECG
- The left chest leads (“left ventricular” complexes in I, aVL, V5, V6) are characterized by qR complexes, and the right chest leads (“right ventricular” complexes in QRS in aVR, V1, V2) are characterized by complexes of the rS type.
R wave height
- Normally, there is a gradual increase from V1 to V5 (“R wave progression”). Max R in V5, less often in V4.
- Lead I ≤ 15 mm (1.5 mV).
- II, III, aVF ≤ 19 mm (1.9 mV)
- V1: years – 0-15 mm, years – 0-8 mm, over 30 years – 0-6 mm
- V2 – 0.3-12 mm (age > 30 years);
- V3 – 3-24 mm (age > 30 years)
- V4-V5 ≤mm (2.5 mV). R in V6 is often lower than in V5.
Transition zone
Typical morphology of the QRS complex in the precordial leads
S wave
It is the deepest negative wave on the ECG. It gradually decreases from V1 to V6; in leads V5, V6 it may be normally absent.
- I, II, aVF ≤ 5 mm (0.5 mV)
- In V3 max - 20 mm (2.0 mV).
- V1 ≥ 3 mm. The depth should not exceed 30 mm, in in rare cases a depth of more than 30 mm is observed in young men.
ST segment
The QRS complex ends with the J point (ST junction), the junction point of the ST segment. The ST segment is located between the J point and the beginning of the T wave and represents the period between the end of depolarization and the beginning of ventricular repolarization. Must be on an isoline, i.e. on the same level as the TR segment.
- leads from the limbs up to 1 mm,
- V1-V2 up to 3 mm,
- V5-V6 up to 2 mm.
- Normal in limb leads up to 0.5 mm
- V1-V2 ≥ 0.5 mm – deviation from the norm
T wave
QRS concordant, except V1-V2
QT interval
Corrected QT value:
- Bazett formula QTc=QT/√RR interval (s)
- Bazett formula modified by Hodges QTc=QT+0.00175 (ventricular rate-60)
Corrected QT<460 мс.
U wave
Examples of a normal ECG
Read also
Sex and sudden cardiac death
Oxygen in myocardial infarction. Impact on mortality
Canakinumab. Impact of cardiovascular risk
Flu. Misconceptions and reality
Homeopathy. Food for thought.
Toxic synovitis. Patient Information
About the verdict to the doctor Elena Misyurina
NSAIDs in the prevention of UTIs
Bronchial asthma. Underestimation and consequences
Alirocumab
Description Alirocumab belongs to the pharmacological group of monoclonal antibodies. This drug is used in the treatment of hypercholesterolemic conditions in patients with serious diseases.
Creutzfeldt-Jakob disease
Creutzfeldt-Jakob disease (H.G. Creutzfeldt, German neurologist and psychiatrist; A. Jakob, German neurologist, corticostriospinal degeneration, spastic pseudosclerosis) is a disease from the medical group.
Prion
PRION is a virus-like particle, an infectious protein, the action of which is attributed to the so-called slow viral diseases, including chicken, Creutzfeldt-Jakob disease, scrapie (sheep scabies), etc.
ECG interpretation, normal indicators
Decoding an ECG is the job of a knowledgeable doctor. This method of functional diagnostics evaluates:
- heart rhythm - the state of the generators of electrical impulses and the state of the heart system conducting these impulses
- the condition of the heart muscle itself (myocardium), the presence or absence of inflammation, damage, thickening, oxygen starvation, electrolyte imbalance
However, modern patients often have access to their medical documents, in particular, to electrocardiography films on which medical reports are written. With their diversity, these recordings can drive even the most balanced but ignorant person to panic disorder. After all, the patient often does not know for certain how dangerous to life and health is what is written on the back of the ECG film by the hand of a functional diagnostician, and there are still several days before an appointment with a therapist or cardiologist.
To reduce the intensity of passions, we immediately warn readers that with not a single serious diagnosis (myocardial infarction, acute rhythm disturbances), a functional diagnostician will not let a patient leave the office, but, at a minimum, will send him for a consultation with a fellow specialist right there. About the rest of the “open secrets” in this article. In all unclear cases of pathological changes in the ECG, ECG monitoring, 24-hour monitoring (Holter), ECHO cardioscopy (ultrasound of the heart) and stress tests (treadmill, bicycle ergometry) are prescribed.
Numbers and Latin letters in ECG interpretation
- When describing an ECG, the heart rate (HR) is usually indicated. The norm is from 60 to 90 (for adults), for children (see table)
- The following are the various intervals and teeth with Latin designations. (ECG with interpretation, see Fig.)
PQ- (0.12-0.2 s) – atrioventricular conduction time. Most often it lengthens against the background of AV blockade. Shortened in CLC and WPW syndromes.
P – (0.1s) height 0.25-2.5 mm describes atrial contractions. May indicate their hypertrophy.
QRS – (0.06-0.1s) -ventricular complex
QT – (no more than 0.45 s) lengthens with oxygen starvation (myocardial ischemia, infarction) and the threat of rhythm disturbances.
RR - the distance between the apices of the ventricular complexes reflects the regularity of heart contractions and makes it possible to calculate heart rate.
The interpretation of the ECG in children is presented in Fig. 3
Heart Rate Description Options
Sinus rhythm
This is the most common inscription found on an ECG. And, if nothing else is added and the frequency (heart rate) is indicated from 60 to 90 beats per minute (for example, heart rate 68`) - this is the best option, indicating that the heart works like a clock. This is the rhythm set by the sinus node (the main pacemaker that generates electrical impulses that cause the heart to contract). At the same time, sinus rhythm implies well-being, both in the state of this node and the health of the conduction system of the heart. The absence of other records denies pathological changes in the heart muscle and means that the ECG is normal. In addition to sinus rhythm, there may be atrial, atrioventricular or ventricular, indicating that the rhythm is set by cells in these parts of the heart and is considered pathological.
Sinus arrhythmia
This is a normal variant in young people and children. This is a rhythm in which impulses leave the sinus node, but the intervals between heart contractions are different. This may be due to physiological changes (respiratory arrhythmia, when heart contractions slow down during exhalation). Approximately 30% of sinus arrhythmias require observation by a cardiologist, as they are at risk of developing more serious rhythm disturbances. These are arrhythmias after rheumatic fever. Against the background of myocarditis or after it, against the background of infectious diseases, heart defects and in persons with a family history of arrhythmias.
Sinus bradycardia
These are rhythmic contractions of the heart with a frequency of less than 50 per minute. In healthy people, bradycardia occurs, for example, during sleep. Bradycardia also often occurs in professional athletes. Pathological bradycardia may indicate sick sinus syndrome. In this case, bradycardia is more pronounced (heart rate from 45 to 35 beats per minute on average) and is observed at any time of the day. When bradycardia causes pauses in heart contractions of up to 3 seconds during the day and about 5 seconds at night, leads to disturbances in the supply of oxygen to tissues and is manifested, for example, by fainting, an operation is indicated to install a cardiac pacemaker, which replaces the sinus node, imposing a normal rhythm of contractions on the heart.
Sinus tachycardia
Heart rate more than 90 per minute is divided into physiological and pathological. In healthy people, sinus tachycardia is accompanied by physical and emotional stress, drinking coffee, sometimes strong tea or alcohol (especially energy drinks). It is short-lived and after an episode of tachycardia, the heart rate returns to normal within a short period of time after stopping the load. With pathological tachycardia, heartbeats bother the patient at rest. Its causes are fever, infections, blood loss, dehydration, thyrotoxicosis, anemia, cardiomyopathy. The underlying disease is treated. Sinus tachycardia is stopped only in case of a heart attack or acute coronary syndrome.
Extarsystole
These are rhythm disturbances in which foci outside the sinus rhythm give extraordinary cardiac contractions, after which there is a pause of twice the length, called compensatory. In general, the patient perceives heartbeats as uneven, rapid or slow, and sometimes chaotic. The most worrying thing is the dips in heart rate. There may be unpleasant sensations in the chest in the form of tremors, tingling, feelings of fear and emptiness in the stomach.
Not all extrasystoles are dangerous to health. Most of them do not lead to significant circulatory disorders and do not threaten either life or health. They can be functional (against the background of panic attacks, cardioneurosis, hormonal imbalances), organic (with ischemic heart disease, heart defects, myocardial dystrophy or cardiopathy, myocarditis). Intoxication and heart surgery can also lead to them. Depending on the place of occurrence, extrasystoles are divided into atrial, ventricular and anthrioventricular (arising in the node at the border between the atria and ventricles).
- Single extrasystoles are most often rare (less than 5 per hour). They are usually functional and do not interfere with normal blood supply.
- Paired extrasystoles, two at a time, accompany a certain number of normal contractions. Such rhythm disturbances often indicate pathology and require further examination (Holter monitoring).
- Allorhythmias are more complex types of extrasystoles. If every second contraction is an extrasystole, this is bigymenia, if every third contraction is trigymenia, every fourth is quadrigymenia.
It is customary to divide ventricular extrasystoles into five classes (according to Lown). They are assessed during daily ECG monitoring, since the readings of a regular ECG in a few minutes may not show anything.
- Class 1 - single rare extrasystoles with a frequency of up to 60 per hour, emanating from one focus (monotopic)
- 2 – frequent monotopic more than 5 per minute
- 3 – frequent polymorphic (of different shapes) polytopic (from different foci)
- 4a – paired, 4b – group (trigymenia), episodes of paroxysmal tachycardia
- 5 – early extrasystoles
The higher the class, the more serious the violations, although today even classes 3 and 4 do not always require drug treatment. In general, if there are less than 200 ventricular extrasystoles per day, they should be classified as functional and not worry about them. For more frequent cases, ECHO CS is indicated, and sometimes cardiac MRI is indicated. It is not the extrasystole that is treated, but the disease that leads to it.
Paroxysmal tachycardia
In general, paroxysm is an attack. A paroxysmal increase in rhythm can last from several minutes to several days. In this case, the intervals between heart contractions will be the same, and the rhythm will increase over 100 per minute (on average from 120 to 250). There are supraventricular and ventricular forms of tachycardia. This pathology is based on abnormal circulation of electrical impulses in the conduction system of the heart. This pathology can be treated. Home remedies to relieve an attack:
- holding your breath
- increased forced cough
- immersing face in cold water
WPW syndrome
Wolff-Parkinson-White syndrome is a type of paroxysmal supraventricular tachycardia. Named after the authors who described it. The appearance of tachycardia is based on the presence of an additional nerve bundle between the atria and ventricles, through which a faster impulse passes than from the main pacemaker.
As a result, an extraordinary contraction of the heart muscle occurs. The syndrome requires conservative or surgical treatment (in case of ineffectiveness or intolerance of antiarrhythmic tablets, during episodes of atrial fibrillation, and with concomitant heart defects).
CLC – syndrome (Clerk-Levi-Christesco)
is similar in mechanism to WPW and is characterized by earlier excitation of the ventricles than normal due to an additional bundle along which the nerve impulse travels. The congenital syndrome is manifested by attacks of rapid heartbeat.
Atrial fibrillation
It can be in the form of an attack or a permanent form. It manifests itself in the form of atrial flutter or fibrillation.
Atrial fibrillation
When flickering, the heart contracts completely irregularly (the intervals between contractions of very different durations). This is explained by the fact that the rhythm is not set by the sinus node, but by other cells of the atria.
The resulting frequency is from 350 to 700 beats per minute. There is simply no full contraction of the atria; contracting muscle fibers do not effectively fill the ventricles with blood.
As a result, the heart’s output of blood deteriorates and organs and tissues suffer from oxygen starvation. Another name for atrial fibrillation is atrial fibrillation. Not all atrial contractions reach the ventricles of the heart, so the heart rate (and pulse) will be either below normal (bradysystole with a frequency of less than 60), or normal (normosystole from 60 to 90), or above normal (tachysystole more than 90 beats per minute ).
An attack of atrial fibrillation is difficult to miss.
- It usually starts with a strong beat of the heart.
- It develops as a series of absolutely irregular heartbeats with a high or normal frequency.
- The condition is accompanied by weakness, sweating, dizziness.
- The fear of death is very pronounced.
- There may be shortness of breath, general agitation.
- Sometimes there is loss of consciousness.
- The attack ends with normalization of the rhythm and the urge to urinate, during which a large amount of urine is released.
To stop an attack, they use reflex methods, drugs in the form of tablets or injections, or resort to cardioversion (stimulating the heart with an electric defibrillator). If an attack of atrial fibrillation is not eliminated within two days, the risks of thrombotic complications (pulmonary embolism, stroke) increase.
With a constant form of heartbeat flicker (when the rhythm is not restored either against the background of drugs or against the background of electrical stimulation of the heart), they become a more familiar companion to patients and are felt only during tachysystole (rapid, irregular heartbeats). The main task when detecting signs of tachysystole of a permanent form of atrial fibrillation on the ECG is to slow down the rhythm to normosystole without trying to make it rhythmic.
Examples of recordings on ECG films:
- atrial fibrillation, tachysystolic variant, heart rate 160 b'.
- Atrial fibrillation, normosystolic variant, heart rate 64 b'.
Atrial fibrillation can develop in the course of coronary heart disease, against the background of thyrotoxicosis, organic heart defects, diabetes mellitus, sick sinus syndrome, and intoxication (most often with alcohol).
Atrial flutter
These are frequent (more than 200 per minute) regular contractions of the atria and equally regular, but less frequent contractions of the ventricles. In general, flutter is more common in the acute form and is better tolerated than flicker, since circulatory disorders are less pronounced. Fluttering develops when:
- organic heart diseases (cardiomyopathies, heart failure)
- after heart surgery
- against the background of obstructive pulmonary diseases
- in healthy people it almost never occurs
Clinically, flutter is manifested by rapid rhythmic heartbeat and pulse, swelling of the neck veins, shortness of breath, sweating and weakness.
Conduction disorders
Normally, having formed in the sinus node, electrical excitation travels through the conduction system, experiencing a physiological delay of a split second in the atrioventricular node. On its way, the impulse stimulates the atria and ventricles, which pump blood, to contract. If in any part of the conduction system the impulse is delayed longer than the prescribed time, then excitation to the underlying sections will come later, and, therefore, the normal pumping work of the heart muscle will be disrupted. Conduction disturbances are called blockades. They can occur as functional disorders, but more often they are the result of drug or alcohol intoxication and organic heart disease. Depending on the level at which they arise, several types are distinguished.
Sinoatrial blockade
When the exit of an impulse from the sinus node is difficult. In essence, this leads to sick sinus syndrome, slowing of contractions to severe bradycardia, impaired blood supply to the periphery, shortness of breath, weakness, dizziness and loss of consciousness. The second degree of this blockade is called Samoilov-Wenckebach syndrome.
Atrioventricular block (AV block)
This is a delay of excitation in the atrioventricular node longer than the prescribed 0.09 seconds. There are three degrees of this type of blockade. The higher the degree, the less often the ventricles contract, the more severe the circulatory disorders.
- In the first, the delay allows each atrial contraction to maintain an adequate number of ventricular contractions.
- The second degree leaves some of the atrial contractions without ventricular contractions. It is described, depending on the prolongation of the PQ interval and the loss of ventricular complexes, as Mobitz 1, 2 or 3.
- The third degree is also called complete transverse blockade. The atria and ventricles begin to contract without interconnection.
In this case, the ventricles do not stop because they obey the pacemakers from the underlying parts of the heart. If the first degree of blockade may not manifest itself in any way and can be detected only with an ECG, then the second is already characterized by sensations of periodic cardiac arrest, weakness, and fatigue. With complete blockades, brain symptoms are added to the manifestations (dizziness, spots in the eyes). Morgagni-Adams-Stokes attacks may develop (when the ventricles escape from all pacemakers) with loss of consciousness and even convulsions.
Impaired conduction within the ventricles
In the ventricles, the electrical signal propagates to the muscle cells through such elements of the conduction system as the trunk of the His bundle, its legs (left and right) and branches of the legs. Blockades can occur at any of these levels, which is also reflected in the ECG. In this case, instead of being simultaneously covered by excitation, one of the ventricles is delayed, since the signal to it bypasses the blocked area.
In addition to the place of origin, a distinction is made between complete or incomplete blockade, as well as permanent and non-permanent blockade. The causes of intraventricular blocks are similar to other conduction disorders (ischemic heart disease, myocarditis and endocarditis, cardiomyopathies, heart defects, arterial hypertension, fibrosis, heart tumors). Also affected are the use of antiarthmic drugs, an increase in potassium in the blood plasma, acidosis, and oxygen starvation.
- The most common is blockade of the anterosuperior branch of the left bundle branch (ALBBB).
- In second place is right leg block (RBBB). This blockade is usually not accompanied by heart disease.
- Left bundle branch block is more typical for myocardial lesions. In this case, complete blockade (PBBB) is worse than incomplete blockade (LBBB). It sometimes has to be distinguished from WPW syndrome.
- Blockade of the posteroinferior branch of the left bundle branch can occur in individuals with a narrow and elongated or deformed chest. Among pathological conditions, it is more typical for overload of the right ventricle (with pulmonary embolism or heart defects).
The clinical picture of blockades at the levels of the His bundle is not expressed. The picture of the underlying cardiac pathology comes first.
- Bailey's syndrome is a two-bundle block (of the right bundle branch and the posterior branch of the left bundle branch).
Myocardial hypertrophy
With chronic overload (pressure, volume), the heart muscle in certain areas begins to thicken, and the chambers of the heart begin to stretch. On the ECG, such changes are usually described as hypertrophy.
- Left ventricular hypertrophy (LVH) is typical for arterial hypertension, cardiomyopathy, and a number of heart defects. But even normally, athletes, obese patients and people engaged in heavy physical labor may experience signs of LVH.
- Right ventricular hypertrophy is an undoubted sign of increased pressure in the pulmonary blood flow system. Chronic cor pulmonale, obstructive pulmonary diseases, cardiac defects (pulmonary stenosis, tetralogy of Fallot, ventricular septal defect) lead to RVH.
- Left atrial hypertrophy (LAH) – with mitral and aortic stenosis or insufficiency, hypertension, cardiomyopathy, after myocarditis.
- Right atrial hypertrophy (RAH) – with cor pulmonale, tricuspid valve defects, chest deformities, pulmonary pathologies and PE.
- Indirect signs of ventricular hypertrophy are deviation of the electrical axis of the heart (EOC) to the right or left. The left type of EOS is its deviation to the left, that is, LVH, the right type is RVH.
- Systolic overload is also evidence of hypertrophy of the heart. Less commonly, this is evidence of ischemia (in the presence of angina pain).
Changes in myocardial contractility and nutrition
Early ventricular repolarization syndrome
Most often, this is a variant of the norm, especially for athletes and people with congenital high body weight. Sometimes associated with myocardial hypertrophy. Refers to the peculiarities of the passage of electrolytes (potassium) through the membranes of cardiocytes and the characteristics of the proteins from which the membranes are built. It is considered a risk factor for sudden cardiac arrest, but does not provide clinical results and most often remains without consequences.
Moderate or severe diffuse changes in the myocardium
This is evidence of a malnutrition of the myocardium as a result of dystrophy, inflammation (myocarditis) or cardiosclerosis. Also, reversible diffuse changes accompany disturbances in water and electrolyte balance (with vomiting or diarrhea), taking medications (diuretics), and heavy physical activity.
Nonspecific ST changes
This is a sign of deterioration in myocardial nutrition without severe oxygen starvation, for example, in the event of an imbalance of electrolytes or against the background of dyshormonal conditions.
Acute ischemia, ischemic changes, T wave changes, ST depression, low T
This describes reversible changes associated with oxygen starvation of the myocardium (ischemia). This can be either stable angina or unstable, acute coronary syndrome. In addition to the presence of the changes themselves, their location is also described (for example, subendocardial ischemia). A distinctive feature of such changes is their reversibility. In any case, such changes require comparison of this ECG with old films, and if a heart attack is suspected, troponin rapid tests for myocardial damage or coronary angiography. Depending on the type of coronary heart disease, anti-ischemic treatment is selected.
Advanced heart attack
It is usually described:
- by stages: acute (up to 3 days), acute (up to 3 weeks), subacute (up to 3 months), cicatricial (all life after a heart attack)
- by volume: transmural (large focal), subendocardial (small focal)
- By location, infarctions are: anterior and anterior septal, basal, lateral, inferior (posterior diaphragmatic), circular apical, posterobasal and right ventricular.
In any case, a heart attack is a reason for immediate hospitalization.
The whole variety of syndromes and specific changes on the ECG, the difference in indicators for adults and children, the abundance of reasons leading to the same type of ECG changes do not allow a non-specialist to interpret even the finished conclusion of a functional diagnostician. It is much wiser, having the ECG result in hand, to visit a cardiologist in a timely manner and receive competent recommendations for further diagnosis or treatment of your problem, significantly reducing the risks of emergency cardiac conditions.
The transcript is incomplete. Not all parameters are specified. In general, before the age of 10, it is better to watch the film. Well, as a last resort, a scan, because... there you need to look at the complexes together. Personally, I prefer to watch “films”; I don’t like reading other people’s protocols. And so, based on these pieces of information, it seems to be within the age norm.
Please decipher the electrocardiogram. Rhythm syn. heart rate 62/m deviation.o.s. left violation proc.ropol. at high levels lateral st.l.zh.
As often happens, not all information is available. By the way, indicating the gender and age of the patient is a must! It appears that we are talking about an elderly patient suffering from chronic ischemic heart disease.
Hello! Please decipher the ECG. Heart rate-77.RV5/SV1 Amplitude 1.178/1. 334mV. P duration/PR Interval 87/119ms Rv5+sv1 Amplitude 2.512mV QRS duration 86ms RV6/SV2 Amplitude 0.926/0.849mv. QTC interval 361/399ms.P/QRS/T angle 71/5/14°
Good afternoon, please help me with decoding the ECG: age 35 years.
You have to look there. It looks like either some kind of intracardiac blockade against the background of sinus (supraventricular) tachycardia, or serious errors in measuring intervals.
Hello! Help me decipher the cardiogram (I’m 37 years old) by writing in “simple language”:
Reduced voltage. The rhythm is sinus, regular heart rate is 64 beats per minute.
EOS is located horizontally. QT prolongation. Pronounced diffuse metabolic changes in the myocardium.
Not a heart, but a Swiss Watch, everything is fine
Hello! Help me decipher 7 years old. Sinus rhythm, heart rate - 92 bpm, EOS - NORMAL POSITION, RBBB, pQ - 0.16 m.sec, QT - 0.34 msec.
The child has an incomplete blockade of the right bundle branch (sometimes normal). In general, everything is within normal limits.
Hello, Help me decipher the cardiogram, I am 55 years old, my blood pressure is normal, I have no diseases.
Heart rate 63 beats/min
PR interval 152 ms
QRS complex 95 ms
QT/QTc 430/441 ms
P/QRS/T axis (deg) 51.7 / 49.4 / 60.8
R(V5) / S(V) 0.77 / 1.07 mV
There is an expansion of the P complex. Either intra-atrial block or hypertrophy of the left atrium. Moderately reduced voltage in the chest leads, if calculated correctly. Not the norm. It is advisable to perform an echocardiogram, because you need to look at the cavity dimensions of the heart and the structure of the myocardium. Cardiosclerosis may be suspected against the background of dilated atria. This often happens with coronary artery disease or after suffering from myocarditis (which, as a complication of acute infections, occurs more often than is commonly thought).
Sinus arrhythmia. A. in stage I blockade. Semi-horizontal EPS. Incomplete blockade of the left leg of the His. Change in/prev. conductivity. Enlargement of the left chambers of the heart.
Male 41 years old. Is consultation with a cardiologist required?
You should definitely consult a cardiologist. For such a not old man, somehow everything is not very good... He’s too young!
Sinus arrhythmia HR = 73 beats/min
EOS is located normally,
Disruption of repolarization processes and decreased myocardial trophism (antero-apical sections).
Help me decipher the cardiogram: sinus rhythm, RBBB.
Male, 26 years old. Is consultation with a cardiologist required? Is treatment required?
Hello! Please tell me if, according to Holter kg per day, in a 12-year-old child, against the background of sinus rhythm, episodes of pacemaker migration at rest, in the daytime with a tendency to bradycardia were recorded. Supraventricular and ventricular activity was recorded, 2 episodes of NVT with aberrant conduction with chssuzh. per minute, episodes of 1st degree AV block, QT 0.44-0.51, can he play sports and what are the risks?
Professional sports, I think, are not desirable. All these phenomena themselves are quite typical for autonomic dysfunction. Dosed physical activity, within reasonable limits, is desirable. In general, the question about sports was asked poorly, not specifically. In this case, based only on the data of daily ECG monitoring according to Holter (which, of course, is not enough), I would not recommend playing sports in conditions with altered partial pressure of oxygen (scuba diving, mountain hiking, parachute jumping) or increased intrathoracic pressure, so-called isometric loads (weightlifting, etc.). The skill level of the trainer is very important in order to correctly calculate the training load regime.
What does it mean? At night, 2 pauses of more than 200 ms (2054 and 2288 ms) were recorded due to the loss of QRST.
I advise you to discuss this issue with a cardiologist. It could be sino-auricular block, with sinus node dysfunction syndrome... Or maybe it’s just a defect in recording or deciphering the recording. In short, consult your doctor. This can be either a small thing or a serious problem.
Hello. Passed the commission. Girl 13 years old.
conclusion: sinus arrhythmia with heart rate min. bradysystole, rhythm with pronounced irregularity, heart rate = 57 beats/min, RR: 810 msms. normal position of the electrical axis of the heart. A passing phenomenon of WPW. RRav = 1054ms RRmin = 810ms RRmax = 1138. Interval: PQ = 130ms. Duration: P=84ms, QRS=90ms, QT=402ms QTcor=392ms
conclusion: migration of the pacemaker through the atria, heart rate 73 per minute. Normosystole, rhythm with pronounced irregularity, heart rate = 73 beats/min, RR: 652ms -1104ms. The PQRST form is a variant of the norm. normal position of the electrical axis of the heart. RRav = 808ms RRmin = 652ms RRmax = 1108. Interval: PQ = 140ms. Duration: P=88ms, QRS=82ms, QT=354ms QTcore=394ms.
There were no problems before. What could it be?
Progrostic mycocarditis of heart valve cysts
First, the interpretation itself raises questions. The average heart rate should be about min., which is normal. Severe sinus arrhythmia in adolescence requires attention, but can also be a normal variant. You need to consult a cardiologist. Does not indicate the type of load applied. There is no normal consideration of the transient phenomenon of ERV. Actually, it is this point that raises the most questions. In short, there are no special disasters, but there are risk factors for arrhythmias. It is advisable for a cardiologist to consider how serious this is. It would be a good idea to come to him with a 24-hour Holter monitoring protocol.
Thank you
The site provides reference information for informational purposes only. Diagnosis and treatment of diseases must be carried out under the supervision of a specialist. All drugs have contraindications. Consultation with a specialist is required!
Electrocardiogram is a widely used method of objective diagnostics various pathologies of the human heart, which is used almost everywhere today. An electrocardiogram (ECG) is taken in a clinic, in an ambulance, or in a hospital department. ECG is a very important recording that reflects the condition of the heart. That is why the reflection of various types of cardiac pathology on the ECG is described by a separate science - electrocardiography. Electrocardiography also deals with the problems of correct ECG recording, decoding issues, interpretation of controversial and unclear points, etc.Definition and essence of the method
An electrocardiogram is a recording of the heart, which is presented as a curved line on paper. The cardiogram line itself is not chaotic; it has certain intervals, teeth and segments that correspond to certain stages of the heart.To understand the essence of an electrocardiogram, you need to know what exactly is recorded by a device called an electrocardiograph. The ECG records the electrical activity of the heart, which changes cyclically in accordance with the onset of diastole and systole. The electrical activity of the human heart may seem like fiction, but this unique biological phenomenon exists in reality. In reality, the heart contains so-called cells of the conduction system, which generate electrical impulses that are transmitted to the muscles of the organ. It is these electrical impulses that cause the myocardium to contract and relax with a certain rhythm and frequency.
The electrical impulse propagates through the cells of the conduction system of the heart strictly sequentially, causing contraction and relaxation of the corresponding sections - the ventricles and atria. The electrocardiogram reflects precisely the total electrical potential difference in the heart.
decryption?
 An electrocardiogram can be taken in any clinic or multidisciplinary hospital. You can contact a private medical center where there is a specialist cardiologist or therapist. After recording the cardiogram, the tape with curves is examined by the doctor. It is he who analyzes the recording, deciphers it and writes a final report, which reflects all visible pathologies and functional deviations from the norm.
An electrocardiogram can be taken in any clinic or multidisciplinary hospital. You can contact a private medical center where there is a specialist cardiologist or therapist. After recording the cardiogram, the tape with curves is examined by the doctor. It is he who analyzes the recording, deciphers it and writes a final report, which reflects all visible pathologies and functional deviations from the norm. An electrocardiogram is recorded using a special device - an electrocardiograph, which can be multi-channel or single-channel. The speed of ECG recording depends on the modification and modernity of the device. Modern devices can be connected to a computer, which, with a special program, will analyze the recording and issue a final conclusion immediately after the procedure is completed.
Any cardiograph has special electrodes that are applied in a strictly defined order. There are four clothespins in red, yellow, green and black that are placed on both arms and both legs. If you go in a circle, then the clothespins are applied according to the rule “red-yellow-green-black”, from the right hand. It's easy to remember this sequence thanks to the student saying: "Every-Woman is an Eviler Trait." In addition to these electrodes, there are also chest electrodes, which are installed in the intercostal spaces.
As a result, the electrocardiogram consists of twelve waveforms, six of which are recorded from the chest electrodes, and are called chest leads. The remaining six leads are recorded from electrodes attached to the arms and legs, with three of them called standard and three more called enhanced. The chest leads are designated V1, V2, V3, V4, V5, V6, the standard ones are simply Roman numerals - I, II, III, and the reinforced leg leads - the letters aVL, aVR, aVF. Different leads of the cardiogram are necessary to create the most complete picture of the activity of the heart, since some pathologies are visible on the chest leads, others on the standard ones, and still others on the enhanced ones.
The person lies down on the couch, the doctor attaches the electrodes and turns on the device. While the ECG is being written, the person must be absolutely calm. We must not allow the appearance of any irritants that can distort the true picture of the work of the heart.
How to correctly perform an electrocardiogram followed by
transcript - video
The principle of decoding an ECG
Since the electrocardiogram reflects the processes of contraction and relaxation of the myocardium, it is possible to trace how these processes occur and identify existing pathological processes. The elements of the electrocardiogram are closely related and reflect the duration of the phases of the cardiac cycle - systole and diastole, that is, contraction and subsequent relaxation. Decoding the electrocardiogram is based on the study of the teeth, their position relative to each other, duration, and other parameters. The following elements of the electrocardiogram are studied for analysis:1. Teeth.
2. Intervals.
3. Segments.
All sharp and smooth convexities and concavities on the ECG line are called teeth. Each tooth is designated by a letter of the Latin alphabet. The P wave reflects contraction of the atria, the QRS complex – contraction of the ventricles of the heart, the T wave – relaxation of the ventricles. Sometimes after the T wave on the electrocardiogram there is another U wave, but it has no clinical and diagnostic role.
An ECG segment is considered to be a segment enclosed between adjacent teeth. For diagnosing heart pathology, the P – Q and S – T segments are of great importance. The interval on the electrocardiogram is a complex that includes a tooth and an interval. The P–Q and Q–T intervals are of great importance for diagnosis.
Often in the doctor’s report you can see small Latin letters, which also indicate teeth, intervals and segments. Small letters are used if the prong is less than 5 mm long. In addition, several R waves may appear in the QRS complex, which are usually designated R’, R”, etc. Sometimes the R wave is simply missing. Then the entire complex is designated by only two letters - QS. All this has important diagnostic significance.
ECG interpretation plan - general scheme for reading results
 When deciphering an electrocardiogram, the following parameters reflecting the work of the heart must be established:
When deciphering an electrocardiogram, the following parameters reflecting the work of the heart must be established: - position of the electrical axis of the heart;
- determining the correctness of the heart rhythm and conductivity of the electrical impulse (blockades, arrhythmias are identified);
- determining the regularity of contractions of the heart muscle;
- determination of heart rate;
- identifying the source of the electrical impulse (whether sinus rhythm is determined or not);
- analysis of the duration, depth and width of the atrial P wave and the P – Q interval;
- analysis of the duration, depth, width of the QRST ventricular wave complex;
- analysis of parameters of the RS – T segment and T wave;
- analysis of Q – T interval parameters.
In the conclusion on the electrocardiogram, the doctor must reflect the following parameters:
- sinus rhythm or not;
- rhythm regularity;
- heart rate (HR);
- position of the electrical axis of the heart.
Example of deciphering an electrocardiogram
At the very beginning of the electrocardiogram tape there should be a calibration signal, which looks like a large letter “P” 10 mm high. If this calibration signal is not present, then the electrocardiogram is uninformative. If the height of the calibration signal is below 5 mm in standard and enhanced leads, and below 8 mm in chest leads, then there is a low voltage of the electrocardiogram, which is a sign of a number of heart pathologies. For subsequent decoding and calculation of some parameters, you need to know what period of time fits into one cell of graph paper. At a belt speed of 25 mm/s, one cell 1 mm long is equal to 0.04 seconds, and at a speed of 50 mm/s – 0.02 seconds.Checking the regularity of heart contractions
It is assessed by the intervals R - R. If the teeth are located at the same distance from each other throughout the entire recording, then the rhythm is regular. Otherwise it is called correct. Estimating the distance between the R - R teeth is very simple: the electrocardiogram is recorded on graph paper, which makes it easy to measure any gaps in millimeters.Heart rate (HR) calculation
 It is carried out using a simple arithmetic method: count the number of large squares on graph paper that are placed between two R waves. Then the heart rate is calculated using the formula, which is determined by the speed of the tape in the cardiograph:
It is carried out using a simple arithmetic method: count the number of large squares on graph paper that are placed between two R waves. Then the heart rate is calculated using the formula, which is determined by the speed of the tape in the cardiograph: 1. The tape speed is 50 mm/s - then the heart rate is 600 divided by the number of squares.
2. The tape speed is 25 mm/s - then the heart rate is 300 divided by the number of squares.
For example, if 4.8 large squares fit between two R teeth, then the heart rate, at a belt speed of 50 mm/s, will be equal to 600/4.8 = 125 beats per minute.
If the heart rate is abnormal, then the maximum and minimum heart rate is determined, also taking as a basis the maximum and minimum distances between the R waves.
Identifying the source of the rhythm
The doctor studies the rhythm of heart contractions and finds out which node of nerve cells causes the cyclic processes of contraction and relaxation of the heart muscle. This is very important for identifying blockages.Decoding ECG - rhythms
Normally, the pacemaker is the sinus node. And such a normal rhythm itself is called sinus - all other options are pathological. In various pathologies, any other node of the nerve cells of the cardiac conduction system can act as a pacemaker. In this case, the cyclic electrical impulses become confused and the heart rhythm is disrupted - arrhythmia occurs.In sinus rhythm on the electrocardiogram in lead II there is a P wave before each QRS complex, and it is always positive. In one lead, all P waves should have the same shape, length and width.
With atrial rhythm the P wave in leads II and III is negative, but is present before each QRS complex.
Atrioventricular rhythms are characterized by the absence of P waves on cardiograms, or the appearance of this wave after the QRS complex, and not before it, as is normal. With this type of rhythm, the heart rate is low, ranging from 40 to 60 beats per minute.
Ventricular rhythm characterized by an increase in the width of the QRS complex, which becomes large and quite frightening. The P waves and the QRS complex are completely unrelated to each other. That is, there is no strict correct normal sequence - the P wave, followed by the QRS complex. Ventricular rhythm is characterized by a decrease in heart rate - less than 40 beats per minute.
Detection of pathology of electrical impulse conduction through the structures of the heart
To do this, measure the duration of the P wave, the P–Q interval and the QRS complex. The duration of these parameters is calculated from the millimeter tape on which the cardiogram is recorded. First, count how many millimeters each tooth or interval occupies, after which the resulting value is multiplied by 0.02 at a recording speed of 50 mm/s, or by 0.04 at a recording speed of 25 mm/s.The normal duration of the P wave is up to 0.1 seconds, the P – Q interval is 0.12-0.2 seconds, the QRS complex is 0.06-0.1 seconds.
Electrical axis of the heart
 Denoted as the alpha angle. It can have a normal position, horizontal or vertical. Moreover, in a thin person the axis of the heart is more vertical relative to the average values, while in a fat person it is more horizontal. The normal position of the electrical axis of the heart is 30–69 o, vertical – 70–90 o, horizontal – 0–29 o. The alpha angle, equal to 91 to ±180 o, reflects a sharp deviation of the electrical axis of the heart to the right. The alpha angle, equal to 0 to –90 o, reflects a sharp deviation of the electrical axis of the heart to the left.
Denoted as the alpha angle. It can have a normal position, horizontal or vertical. Moreover, in a thin person the axis of the heart is more vertical relative to the average values, while in a fat person it is more horizontal. The normal position of the electrical axis of the heart is 30–69 o, vertical – 70–90 o, horizontal – 0–29 o. The alpha angle, equal to 91 to ±180 o, reflects a sharp deviation of the electrical axis of the heart to the right. The alpha angle, equal to 0 to –90 o, reflects a sharp deviation of the electrical axis of the heart to the left. The electrical axis of the heart can deviate under various pathological conditions. For example, hypertension leads to a deviation to the right; a conduction disorder (blockade) can shift it to the right or left.
Atrial P wave
The atrial P wave should be:- positive in I, II, aVF and chest leads (2, 3,4, 5, 6);
- negative in aVR;
- biphasic (part of the tooth lies in the positive region, and part in the negative) in III, aVL, V1.
Pathological forms of the P wave may indicate the following pathologies:
1.
Tall and sharp teeth in leads II, III, aVF appear with hypertrophy of the right atrium (“cor pulmonale”);
2.
A P wave with two peaks and a large width in leads I, aVL, V5 and V6 indicates hypertrophy of the left atrium (for example, mitral valve disease).
P–Q interval
The P–Q interval has a normal duration of 0.12 to 0.2 seconds. An increase in the duration of the P–Q interval is a reflection of atrioventricular block. On the electrocardiogram, three degrees of atrioventricular block (AV) can be distinguished:- I degree: simple lengthening of the P–Q interval while maintaining all other complexes and waves.
- II degree: prolongation of the P–Q interval with partial loss of some QRS complexes.
- III degree: lack of connection between the P wave and QRS complexes. In this case, the atria work in their own rhythm, and the ventricles - in their own.
Ventricular QRST complex
 The ventricular QRST complex consists of the QRS complex itself and the S – T segment. The normal duration of the QRST complex does not exceed 0.1 seconds, and its increase is detected with blockades of the Hiss bundle branches.
The ventricular QRST complex consists of the QRS complex itself and the S – T segment. The normal duration of the QRST complex does not exceed 0.1 seconds, and its increase is detected with blockades of the Hiss bundle branches. QRS complex consists of three waves, Q, R and S, respectively. The Q wave is visible on the cardiogram in all leads except 1, 2 and 3 chest leads. A normal Q wave has an amplitude up to 25% of that of an R wave. The duration of the Q wave is 0.03 seconds. The R wave is recorded in absolutely all leads. The S wave is also visible in all leads, but its amplitude decreases from the 1st thoracic to the 4th, and in the 5th and 6th it may be completely absent. The maximum amplitude of this tooth is 20 mm.
The S–T segment is very important from a diagnostic point of view. It is by this tooth that myocardial ischemia can be detected, that is, a lack of oxygen in the heart muscle. Usually this segment runs along the isoline, in the 1st, 2nd and 3rd chest leads; it can rise up by a maximum of 2 mm. And in the 4th, 5th and 6th chest leads, the S-T segment can shift below the isoline by a maximum of half a millimeter. It is the deviation of the segment from the isoline that reflects the presence of myocardial ischemia.
T wave
The T wave is a reflection of the process of eventual relaxation in the cardiac muscle of the ventricles of the heart. Typically, when the amplitude of the R wave is large, the T wave will also be positive. A negative T wave is normally recorded only in lead aVR.Q-T interval
The Q–T interval reflects the process of eventual contraction in the myocardium of the ventricles of the heart.ECG interpretation - normal indicators
The transcript of the electrocardiogram is usually recorded by the doctor in conclusion. A typical example of a normal cardiac cardiogram looks like this:1. PQ – 0.12 s.
2. QRS – 0.06 s.
3. QT – 0.31 s.
4. RR – 0.62 – 0.66 – 0.6.
5. Heart rate is 70 - 75 beats per minute.
6. sinus rhythm.
7. The electrical axis of the heart is located normally.
Normally, the rhythm should be only sinus, the heart rate of an adult is 60 - 90 beats per minute. The P wave is normally no more than 0.1 s, the P – Q interval is 0.12-0.2 seconds, the QRS complex is 0.06-0.1 seconds, Q – T is up to 0.4 s.
If the cardiogram is pathological, then it indicates specific syndromes and deviations from the norm (for example, partial blockade of the left bundle branch, myocardial ischemia, etc.). The doctor can also reflect specific violations and changes in the normal parameters of the waves, intervals and segments (for example, shortening of the P wave or Q-T interval, etc.).
Interpretation of ECG in children and pregnant women
In principle, children and pregnant women have normal heart electrocardiogram readings - the same as in healthy adults. However, there are certain physiological characteristics. For example, the heart rate of children is higher than that of an adult. The normal heart rate of a child up to 3 years of age is 100–110 beats per minute, 3–5 years old – 90–100 beats per minute. Then gradually the heart rate decreases, and in adolescence it is compared with that of an adult - 60 - 90 beats per minute.In pregnant women, there may be a slight deviation of the electrical axis of the heart in late gestation due to compression by the growing uterus. In addition, sinus tachycardia often develops, that is, an increase in heart rate to 110 - 120 beats per minute, which is a functional condition and goes away on its own. An increase in heart rate is associated with a greater volume of circulating blood and increased workload. Due to the increased load on the heart, pregnant women may experience overload in various parts of the organ. These phenomena are not a pathology - they are associated with pregnancy and will go away on their own after childbirth.
Decoding the electrocardiogram during a heart attack
 Myocardial infarction is a sudden cessation of oxygen supply to the heart muscle cells, resulting in the development of necrosis of a tissue area that is in a state of hypoxia. The reason for the disruption of oxygen supply can be different - most often it is a blockage of a blood vessel, or its rupture. A heart attack involves only part of the muscle tissue of the heart, and the extent of the damage depends on the size of the blood vessel that is blocked or ruptured. On an electrocardiogram, myocardial infarction has certain signs by which it can be diagnosed.
Myocardial infarction is a sudden cessation of oxygen supply to the heart muscle cells, resulting in the development of necrosis of a tissue area that is in a state of hypoxia. The reason for the disruption of oxygen supply can be different - most often it is a blockage of a blood vessel, or its rupture. A heart attack involves only part of the muscle tissue of the heart, and the extent of the damage depends on the size of the blood vessel that is blocked or ruptured. On an electrocardiogram, myocardial infarction has certain signs by which it can be diagnosed. In the process of development of myocardial infarction, four stages are distinguished, which have different manifestations on the ECG:
- acute;
- acute;
- subacute;
- cicatricial.
Sometimes it is possible to detect the phase of myocardial ischemia preceding the acute phase, which is characterized by high T waves.
Acute stage A heart attack lasts 2–3 weeks. During this period, a wide and high-amplitude Q wave and a negative T wave are recorded on the ECG.
Subacute stage lasts up to 3 months. The ECG shows a very large negative T wave with a huge amplitude, which gradually normalizes. Sometimes a rise in the S-T segment is detected, which should have leveled off by this period. This is an alarming symptom, as it may indicate the formation of a cardiac aneurysm.
Scar stage heart attack is final, since connective tissue that is unable to contract is formed at the damaged site. This scar is recorded on the ECG as a Q wave, which will remain for life. Often the T wave is smoothed, has a low amplitude, or is completely negative.
Interpretation of the most common ECGs
 In conclusion, doctors write the result of the ECG interpretation, which is often incomprehensible because it consists of terms, syndromes and simply statements of pathophysiological processes. Let's consider the most common ECG conclusions, which are incomprehensible to a person without a medical education.
In conclusion, doctors write the result of the ECG interpretation, which is often incomprehensible because it consists of terms, syndromes and simply statements of pathophysiological processes. Let's consider the most common ECG conclusions, which are incomprehensible to a person without a medical education. Ectopic rhythm means not sinus - which can be either a pathology or a norm. The norm is ectopic rhythm when there is a congenital malformation of the conduction system of the heart, but the person does not present any complaints and does not suffer from other cardiac pathologies. In other cases, an ectopic rhythm indicates the presence of blockades.
Changes in repolarization processes on the ECG reflects a violation of the process of relaxation of the heart muscle after contraction.
Sinus rhythm This is the normal heart rate of a healthy person.
Sinus or sinusoidal tachycardia means that a person has a correct and regular rhythm, but an increased heart rate - more than 90 beats per minute. In young people under 30 years of age, this is a variant of the norm.
Sinus bradycardia- this is a low heart rate - less than 60 beats per minute against the background of a normal, regular rhythm.
Nonspecific ST-T changes mean that there are minor deviations from the norm, but their cause may be completely unrelated to heart pathology. It is necessary to undergo a full examination. Such nonspecific ST-T changes can develop with an imbalance of potassium, sodium, chlorine, magnesium ions, or various endocrine disorders, often during menopause in women.
Biphasic R wave in combination with other signs of a heart attack indicates damage to the anterior wall of the myocardium. If no other signs of a heart attack are detected, then a biphasic R wave is not a sign of pathology.
QT prolongation may indicate hypoxia (lack of oxygen), rickets, or overexcitation of the child’s nervous system, which is a consequence of birth trauma.
Myocardial hypertrophy means that the muscular wall of the heart is thickened and works under enormous load. This can lead to the formation of:
- heart failure;
- arrhythmias.
Moderate diffuse changes in the myocardium mean that tissue nutrition is impaired and cardiac muscle dystrophy has developed. This is a fixable condition: you need to see a doctor and undergo an adequate course of treatment, including normalizing your diet.
Deviation of the electrical axis of the heart (EOS) left or right is possible with hypertrophy of the left or right ventricle, respectively. EOS can deviate to the left in obese people, and to the right - in thin people, but in this case this is a variant of the norm.
Left type ECG– EOS deviation to the left.
NBPNPG– an abbreviation for “incomplete right bundle branch block.” This condition can occur in newborns and is a normal variant. In rare cases, RBBB can cause arrhythmia, but generally does not lead to the development of negative consequences. Block of the Hiss bundle branch is quite common in people, but if there are no complaints about the heart, then it is not at all dangerous.
BPVLNPG– an abbreviation meaning “blockade of the anterior branch of the left bundle branch.” Reflects a violation of the conduction of electrical impulses in the heart, and leads to the development of arrhythmias.
Small growth of the R wave in V1-V3 may be a sign of interventricular septal infarction. To accurately determine whether this is the case, it is necessary to do another ECG study.
CLC syndrome(Klein-Levy-Kritesco syndrome) is a congenital feature of the conduction system of the heart. May cause the development of arrhythmias. This syndrome does not require treatment, but it is necessary to be regularly examined by a cardiologist.
Low voltage ECG often recorded with pericarditis (a large amount of connective tissue in the heart that has replaced muscle tissue). In addition, this sign may be a reflection of exhaustion or myxedema.
Metabolic changes are a reflection of insufficient nutrition of the heart muscle. It is necessary to be examined by a cardiologist and undergo a course of treatment.
Conduction slowdown means that the nerve impulse travels through the tissues of the heart more slowly than normal. This condition itself does not require special treatment - it may be a congenital feature of the conduction system of the heart. Regular monitoring by a cardiologist is recommended.
Blockade 2 and 3 degrees reflects a serious disturbance of cardiac conduction, which is manifested by arrhythmia. In this case, treatment is necessary.
Rotation of the heart by the right ventricle forward may be an indirect sign of the development of hypertrophy. In this case, it is necessary to find out its cause and undergo a course of treatment, or adjust your diet and lifestyle.
Price of an electrocardiogram with interpretation
The cost of an electrocardiogram with interpretation varies significantly, depending on the specific medical institution. Thus, in public hospitals and clinics the minimum price for the procedure of taking an ECG and interpreting it by a doctor is from 300 rubles. In this case, you will receive films with recorded curves and a doctor’s conclusion on them, which he will make himself, or using a computer program.If you want to receive a thorough and detailed conclusion on the electrocardiogram, a doctor’s explanation of all the parameters and changes, it is better to contact a private clinic that provides such services. Here the doctor will be able not only to write a conclusion by deciphering the cardiogram, but also to calmly talk to you, taking his time to explain all the points of interest. However, the cost of such a cardiogram with interpretation in a private medical center ranges from 800 rubles to 3,600 rubles. You should not assume that bad specialists work in an ordinary clinic or hospital - it’s just that a doctor in a public institution, as a rule, has a very large amount of work, so he simply does not have time to talk with each patient in great detail.
The direction of the electrical axis of the heart depends on many factors (age of the child, hypertrophy of the heart, position of the heart in the chest, etc.). In children 3-14 years old, the electrical axis is within the range of +30° ÷ +70°. In children under 3 years of age, the electrical axis of the heart is in the sector +70° ÷ +100°.
Transition zone. When analyzing an ECG, the transition zone should be taken into account - it is determined by a lead in which the R and S waves are equiphase, i.e. their amplitude on both sides of the isoelectric line is equal. In healthy older children, the QRS transition zone is usually determined in leads V3,4. When the ratio of vector forces changes, the transition zone moves towards their predominance. For example, with right ventricular hypertrophy, the transition zone moves to the position of the left chest electrodes and vice versa. There is a gradual or abrupt formation of the transition zone. The transition zone has no independent significance in diagnosis. For example, with biventricular hypertrophy of the ventricular myocardium, no displacement of the transition zone is observed. However, in combination with other diagnostic signs, the displacement of the transition zone acquires a certain weight.
SI, II, III - ECG type. This designates an ECG that has an S wave in three standard leads, the amplitude of which is equal to or greater than the R amplitude, and a QRS complex of the RS form without a Q wave. In this case, there is often a low-voltage curve and rSRV1. This type of ECG occurs in a small number of observations (0.5 - 1%) in healthy children, relatively often in patients with pneumonia, with some congenital heart defects, etc. SI, II, III - type of ECG, caused by rotation of the heart around the transverse axis apex posteriorly. The diagnostic value of SI, II, III type ECG increases with its sudden appearance.
“Diseases of the heart and blood vessels in children”, N.A. Belokon
